What’s the problem?
Typically, the process for getting any procedure done, such as a colonoscopy, involves a lot of waiting around. This drives anxiety and may lead to a poor patient experience (not good for reimbursement!). However, my recent experience with undergoing a colonoscopy was surprisingly pleasant. Below, I explain why.
Problem Description
They tell you to arrive an hour or two early whenever you need a procedure like a colonoscopy. But you never really know how long the person before you will take, so you might end up waiting two or three hours. This isn’t pleasant, especially since you’re fasting. There’s nothing worse than a hangry patient.
The other day, I had to get a colonoscopy. I’ll spare you the details of the actual procedure, but I’m happy to talk about the process.
A week before the procedure, someone from the endoscopy site called to confirm my appointment. During the call, they asked me some intake questions:
Medical history
Current medications
Allergies
Any adverse reactions to anesthesia
They also went over the prep instructions: drink two whole bottles of Gatorade mixed with Miralax to clear things out.
A few days before the procedure, I received a text from the endoscopy site with the location and time I should arrive. Noted.
On the day of my colonoscopy, I showed up at the stated time, around 2 PM, for my 3 PM procedure. The receptionist upstairs took my insurance card, ID, and copayment. After signing some forms, I was instructed to take the elevator to the basement floor. Interesting—the actual endoscopy suite is in the basement, and the first floor is just the intake area.
When I exited the elevator, there was a beautiful waiting area. I sat down with what looked like family members waiting for their loved ones to finish their procedures. I had just sat down when a nurse opened a door and called my name.
“Jared?”
“Present!”
The nurse greeted me and took me back to a room where I changed into a gown and removed my jewelry. She asked me more specific questions than the intake ones from the week before (e.g., last bowel movement, last time eating). After that, she took my vitals, placed an IV, and started some maintenance fluids. Once she left, the anesthesiologist came in to greet me and ask some anesthesia-specific questions. I signed the consent form and they left. A few minutes later, the gastroenterologist walked in, talked to me about the procedure, and had me sign another consent form. It was literally back to back to back.
By now it was around 2:30 PM. The nurse told me to text my wife and tell her to leave now to pick me up. Looks like I’m going in 30 minutes early! I texted her, and the nurse took my phone. The anesthesiologist rolled me back to the endoscopy suite where the GI doctor and nurse were waiting.
Not even five minutes after I got into the room, the anesthesiologist had me roll to my side, pushed some propofol, and it was lights out.
I woke up in the post-procedure area about 30 minutes later—so now it was around 3:10 PM. The nurse gave me some food, which I ate. She then had me stand up to ensure I could walk and balance myself, which I could. After I changed, she walked me back to the waiting area, where my lovely wife was waiting for me. We took the elevator upstairs, hailed a cab, and returned home. We arrived home by 3:30 PM (30 minutes after my initial procedure start time).
The total time for everything was about an hour and thirty minutes. Impressive, I’d say. I’ve never had such a streamlined experience in the healthcare setting before.
Below, I’ve produced a process map of my journey.
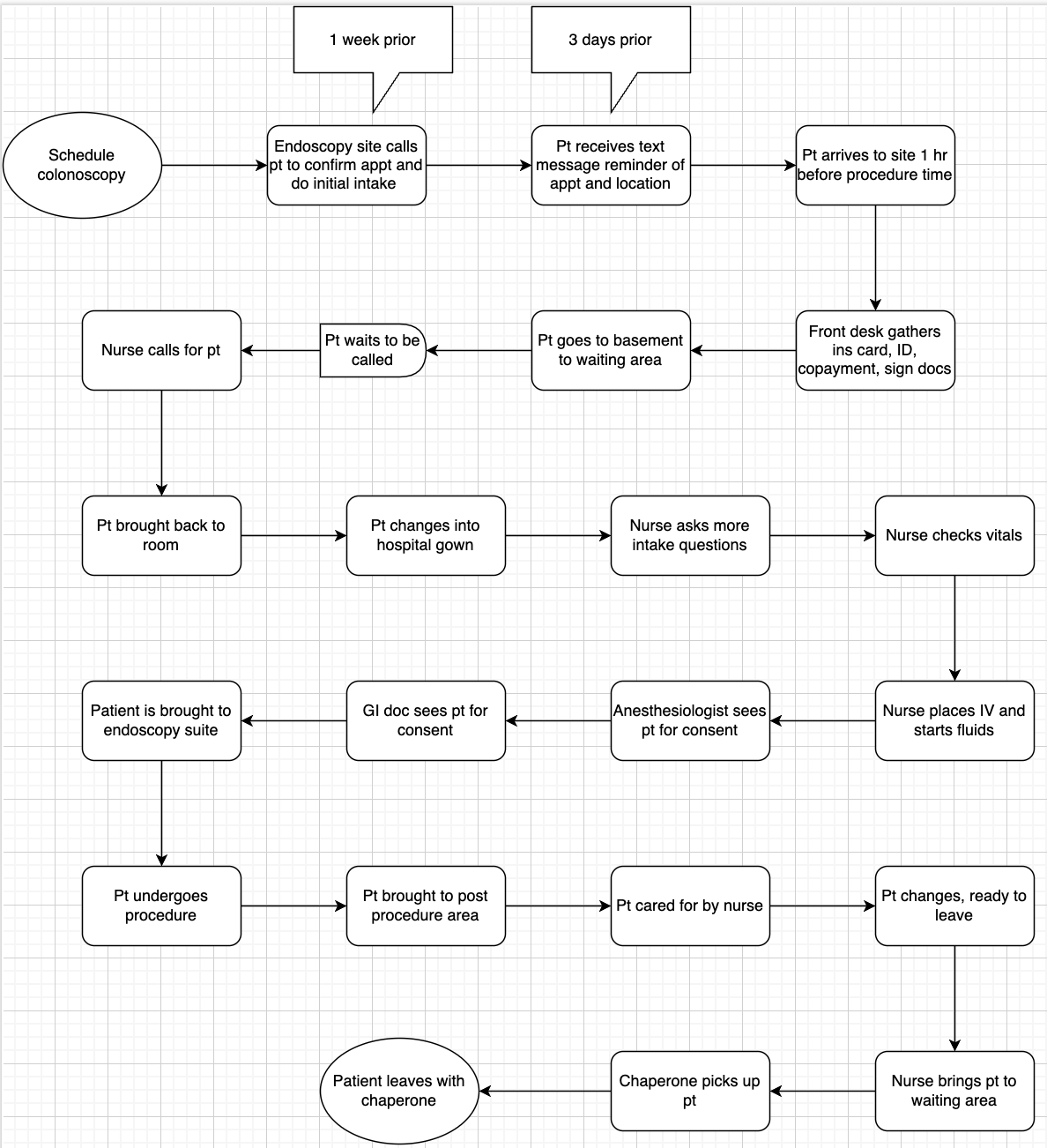
Want to learn about process maps? Click here.
Areas for Improvement
This wasn’t my first rodeo with a colonoscopy, so I knew what to expect. I’ve been on the patient side and physician side of the procedure—which has been quite insightful regarding my analysis of the workflow. However, reflecting on the process, I think if there was one thing to improve on, it would be on the prep experience. If this were my first colonoscopy, I would have definitely been confused and stressed about the prep instructions.
A possible solution? Given the endoscopy site already utilizes patient text messaging, it would be innovative to notify patients of the following as they initiate their colonoscopy prep:
“Good morning! Your colonoscopy is scheduled for 3 PM tomorrow. You can have a light breakfast low in fiber starting now. After 12 PM, you can eat no more solid food. You can have clear liquids, including jello, broth, coffee, etc.”
“Good afternoon! It’s 12 PM. No more solid foods. Please stick to a clear liquid diet.”
“Good evening! It’s 6 PM. You should mix your Miralax and Gatorade now. Begin drinking it. You should start moving your bowels within one to two hours of drinking the mix.”
“Hi! At this point, you should have had several bowel movements, which should be getting clearer.”
“Have a good night's sleep! When you wake up tomorrow, please finish the prep.”
“Good morning! Please finish the rest of your prep. Your bowel movements should be clear here on after.”
“Hi! Checking in. If your bowel movements aren’t clear yet, please give us a call so we can give you further instructions. If they’re clear, we will see you shortly.”
“Good afternoon! We will see you in one hour.”
I just feel like the constant checking-in can help keep patients on track, given poor bowel prep can lead to a wasted colonoscopy.

POLL
How would you describe your colonoscopy workflow experience?

LAST WEEK’S INEFFICIENCY INSIGHTS
You have access to recent Inefficiency Insights here.

HUDDLE #TRENDS
Monthly deep dives into pivotal healthcare trends, crafted as enduring resources for research.
Check out the most recent Huddle #Trends report below 👇
You have access to recent Huddle #Trends reports here.

HUDDLE UNIVERSITY
Click below for my newest course: The Art of Problem-solving in Healthcare.

P.S. Need Huddle+ for your team? Send me an email ([email protected]) for more info about Huddle+ corporate subscriptions and discounts.
Please be advised that the content expressed within 'Inefficiency Insights', including all views and opinions, are solely those of the author and do not represent or reflect the views, policies, or practices of the institution with which the author is affiliated. The inefficiencies and related matters discussed in this newsletter are synthesized from a variety of sources, including but not limited to academic journal articles, generalized patient experiences, and the author's cumulative experiences in the healthcare sector over several years, and should not be construed as specific to or indicative of the practices at the author's place of employment.









