
I see the downstream consequences of primary care failure every day, as an internal medicine resident.
The patient who arrives in the emergency department with decompensated heart failure because nobody caught the 10-pound weight gain two weeks earlier.
The patient with diabetes with an A1c of 11% who hasn't seen a primary care doctor in a year because they couldn't get to their appointment.
The elderly patient who was discharged from the hospital six days ago and hasn't heard from anyone.
I see some version of this every week.
We talk about the primary care workforce shortage in abstract terms—statistics, projections, policy discussions about reimbursement models. From what I see, though, the shortage manifests as a steady stream of patients who slip through the cracks of a system that simply doesn't have the capacity to keep up.
Lumeris’ agentic AI platform, Tom, is the most serious attempt I've seen to rethink what primary care can look like.
In this article, I'll dive into Lumeris and their platform Tom, explore the primary care access crisis, and discuss how this impacts our patients, physicians, and the health system at large.
The Deets: Lumeris and Tom
Who is Lumeris?
Lumeris is a leader in healthcare technology and services with over a decade of experience managing risk for millions of patients alongside major health systems and large medical groups. They also operate Essence Healthcare, a Medicare Advantage plan that consistently earns high Star Quality Ratings.
Most healthcare AI companies are building on theoretical frameworks. Lumeris, however, is building on a decade of data, clinical workflows, and hard-won experience managing complex patient populations at scale.
In early 2025, they introduced Tom—their AI operating system for primary care—and with it, a new category of software they're calling Primary Care as a Service (PCaaS). Named in honor of the late Dr. Tom Doerr, a Lumeris founder and champion of patient-centered primary care, Tom reflects his vision of expanding access and improving healthcare through innovation.
Who (or What) is Tom?
Tom is a multi-agent agentic AI operating system designed to function as a full member of the primary care team—an always-on system that checks in on patient populations, identifies the best next action for each patient, and then takes that action. Tom doesn't replace members of the care team but rather augments the staff, helping to free up capacity to spend more meaningful time with patients.
Lumeris frames it as the "infinite resident." Think of a team of residents (or a bunch of “Jareds”) who are continuously reviewing your panel: flagging the patient whose blood pressure trend looks dangerous, scheduling the follow-up that was supposed to happen two weeks ago, reaching out to the patient who missed their diabetes check-in. That's Tom—working in the background, around the clock, across every patient on the panel.
A few of Tom's core capabilities:
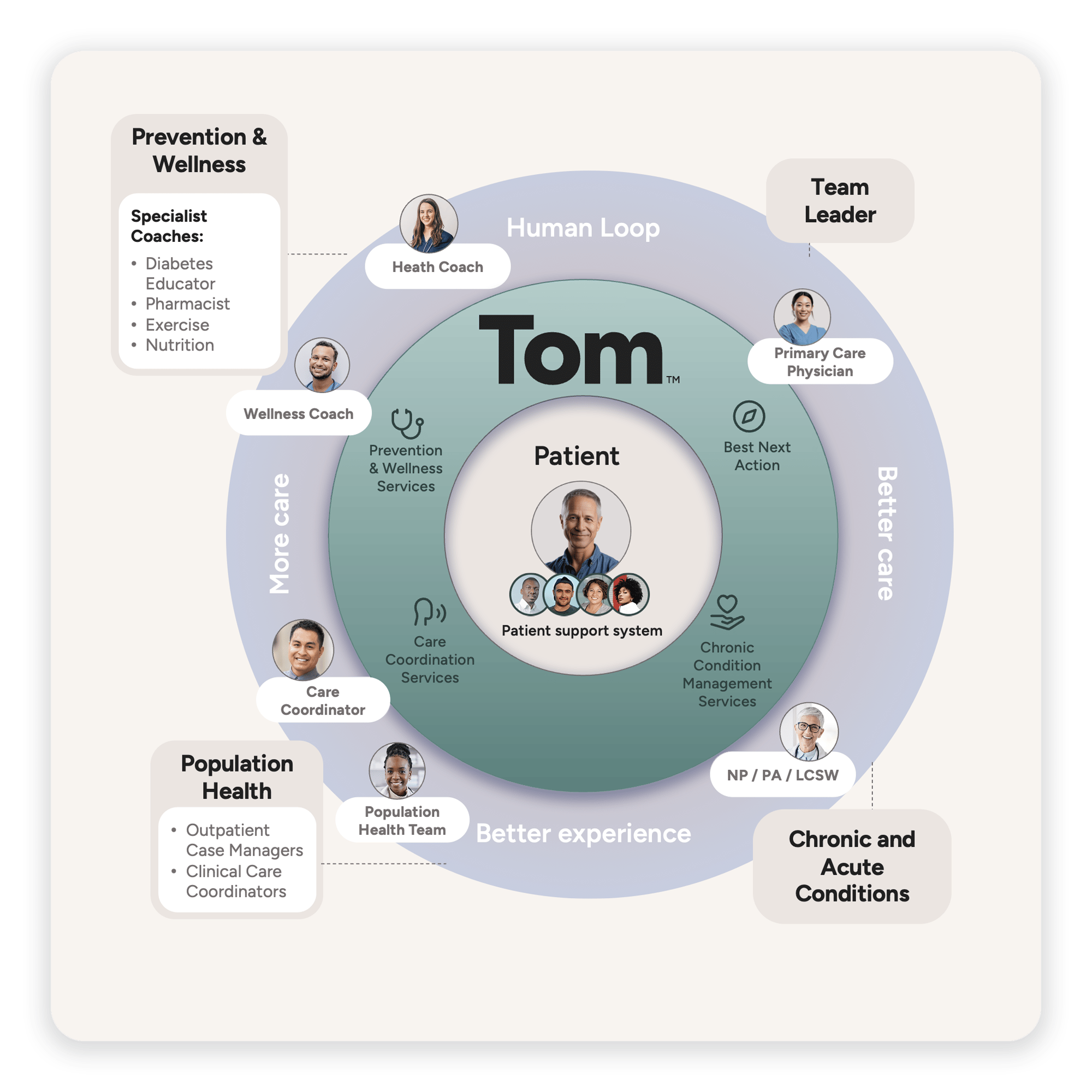
Best Next Action: Tom continuously analyzes patient data to recommend the most impactful intervention for each patient, then executes it autonomously within defined clinical guardrails
Ask Tom: A conversational interface that lets clinicians interact naturally with the system to query population and patient-specific data.
Best Clinical Guidance: Tom sifts through vast amounts of information including conversational information and patient-reported symptoms to make recommendations to the care team, backed by clinical evidence and standards.
Population-level monitoring: Real-time surveillance drawing from EHRs, claims, labs, pharmacies, and wearables.
Automated outreach: Proactive patient engagement for cancer screenings, vaccinations, post-discharge follow-ups, medication adherence, and chronic disease management.
The key distinction from other healthcare AI tools—and Lumeris is emphatic about this—is that Tom is actually filling the care gaps. Most AI platforms in healthcare are still generating a gaps-in-care list and handing it to a human (seriously, I get emailed an excel document of my patient’s care gaps every week). Tom is designed to autonomously close those administrative gaps and escalate to clinical oversight only when required.
The Primary Care Access Problem
Nearly 100 million Americans lack access to primary care. For perspective, that's the entire population of California, New Jersey, New York, and Texas combined—imagine all those people without primary care access! The U.S. is also projected to face a shortage of nearly 90,000 physicians over the next decade. With a rapidly aging population, there will soon be more Americans over 65 than under 18. That demographic shift brings an epidemic of chronic disease: cardiometabolic conditions, cancer, neurocognitive diseases, behavioral health.
You don't need to be an economist to see that demand is rising fast and supply isn't keeping up.
Generative and agentic AI, however, make it possible to scale parts of the primary care workflow—symptom check, follow-ups, care coordination, chronic condition management, population monitoring—in ways that weren't feasible before. That's the opening Lumeris is building into.
How Tom Reimagines Primary Care
The Care Team Model
Tom is designed to function as an additional layer on the primary care team, one that operates continuously in the background, surfaces critical information proactively, and absorbs the administrative and coordination tasks that currently consume enormous physician capacity. Kind of like the “guardian angel tech” I’ve discussed in past articles.
Dr. David Carmouche, Lumeris's chief medical and commercial officer and an internist himself, describes the future this way: primary care transforms from a transactional series of office visits into a continuous ambient monitoring service. "Going to the doctor" becomes "being with the doctor." I actually love that line.
In practice, this looks like:
Wearables and connected devices feed continuous data streams into Tom, which assesses trends in heart rate, sleep, weight, and biometrics to identify early deterioration.
Tom proactively reaches out to patients before crises develop—checking in after hospital discharge, confirming medication adherence, flagging the early warning signs that would previously only surface at an annual visit.
When physical examination is truly necessary, it becomes a high-precision logistical event— deployed deliberately, not reflexively.
For the primary care physician, the workspace looks less like a waiting room schedule and more like a command center. They're reviewing a dynamically prioritized queue of cases Tom has already prepared, spending their clinical hours on the complex patients, the ambiguous presentations, the relationships that require empathy and judgment rather than pattern-matching.
What I Would Have Used This For
During my residency, I've cared for patients who were admitted for complications that a more proactive system might have caught earlier. Look no further than my opening examples about the patient with heart failure who gained 10 pounds over two weeks or the patient with uncontrolled diabetes who hasn’t been seen in a year.
What strikes me about Tom's design, though, is that it's built precisely for those failure modes.
Continuous biometric monitoring that can catch early fluid retention.
Automated outreach to patients who haven't completed scheduled follow-up.
Best Next Action logic that prioritizes the interventions most likely to prevent the admission I'm about to manage.
I've spent a lot of time in my own training thinking about asynchronous care, like ordering labs in advance of appointments, using phone calls and message-based check-ins to manage stable patients between visits. Tom formalizes and scales that workflow in a way no individual clinician can replicate manually across a panel of thousands.
The platform is already being deployed with Ochsner Health as part of their enterprise AI strategy to expand primary care access, including a specific focus on rural health, where the access gap is most severe.
Dashevsky's Dissection
Impact on Patients
For 100 million Americans without primary care access, Tom's most direct impact is making care available. If it enables physicians to manage panels of 5,000 patients instead of 1,500, that's major capacity expansion without new physicians or facilities.
For existing patients, the value is continuity and proactivity—a care team that checks in between visits, intervenes before crises, and connects you to the right resource early.
The caveat: this requires trust. Patients must feel AI interactions connect to a physician who knows them. The goal isn't removing humans from care but making them more present by eliminating administrative noise.
Impact on Physicians
What will drive physician adoption: time.
Primary care physicians are burning out from administrative work—documentation, care gap management, inbox overflow, follow-up coordination. These tasks consume hours daily and require minimal clinical judgment.
If Tom absorbs that burden, the physician's day transforms. They practice at the top of their license, handling complex cases, ambiguous presentations, and relationships requiring judgment and empathy.
For newer practitioners: real-time clinical nudges and evidence-based recommendations embedded in workflow.
Impact on Health Systems
Health system leaders face extraordinary financial pressure in primary care. Tom's business case addresses multiple priorities.
Panel expansion means more patients per physician, driving value-based contract revenue. Proactive monitoring reduces expensive downstream utilization—hospitalizations, avoidable ED visits, specialist referrals. Keepage improves as Tom coordinates in-network referrals, capturing more total medical spend.
Lumeris brings what most healthcare AI startups lack: a decade of risk management experience. Tom is built with that operational context—not theoretical—shaped by managing risk for millions of patients.
That distinction matters when executives evaluate trusting a new AI platform with primary care infrastructure.
In summary, Tom represents a structural solution to the primary care access crisis. It's designed as infrastructure that reorganizes care delivery, not just another point solution. For health systems expanding access without adding physicians, and for clinicians wanting to focus on work requiring clinical judgment, this is the direction primary care needs to move.






