Early-Onset Colorectal Cancer: 2026 Stats and How to Screen
Colorectal cancer (CRC) is rising among adults under 50—and it's now the leading cause of cancer-related deaths in this age group in the U.S. I'd call this a public health crisis that's been brewing for decades, perhaps a bit under the radar, only now showing itself to us.
While we're actually seeing progress in older age groups, this trend (rising CRC) is accelerating in younger adults. It’s worth talking about.
In this article, I dive into the latest paper from the American Cancer Society reporting new stats and projections on CRC. I'll highlight how we can use technology and robust screening tools to address this troubling trend, and explore how this impacts stakeholders in healthcare (pretty obvious, but worth reiterating).
A Troubling Trend: CRC in People 50 and Younger
While colorectal cancer incidence and mortality have steadily declined in adults 65 and older (driven by screening and treatment advances), rates are rising in those under 65—most alarmingly in those under 50.
CRC is now the number one cause of cancer death in adults under 50 in the U.S.
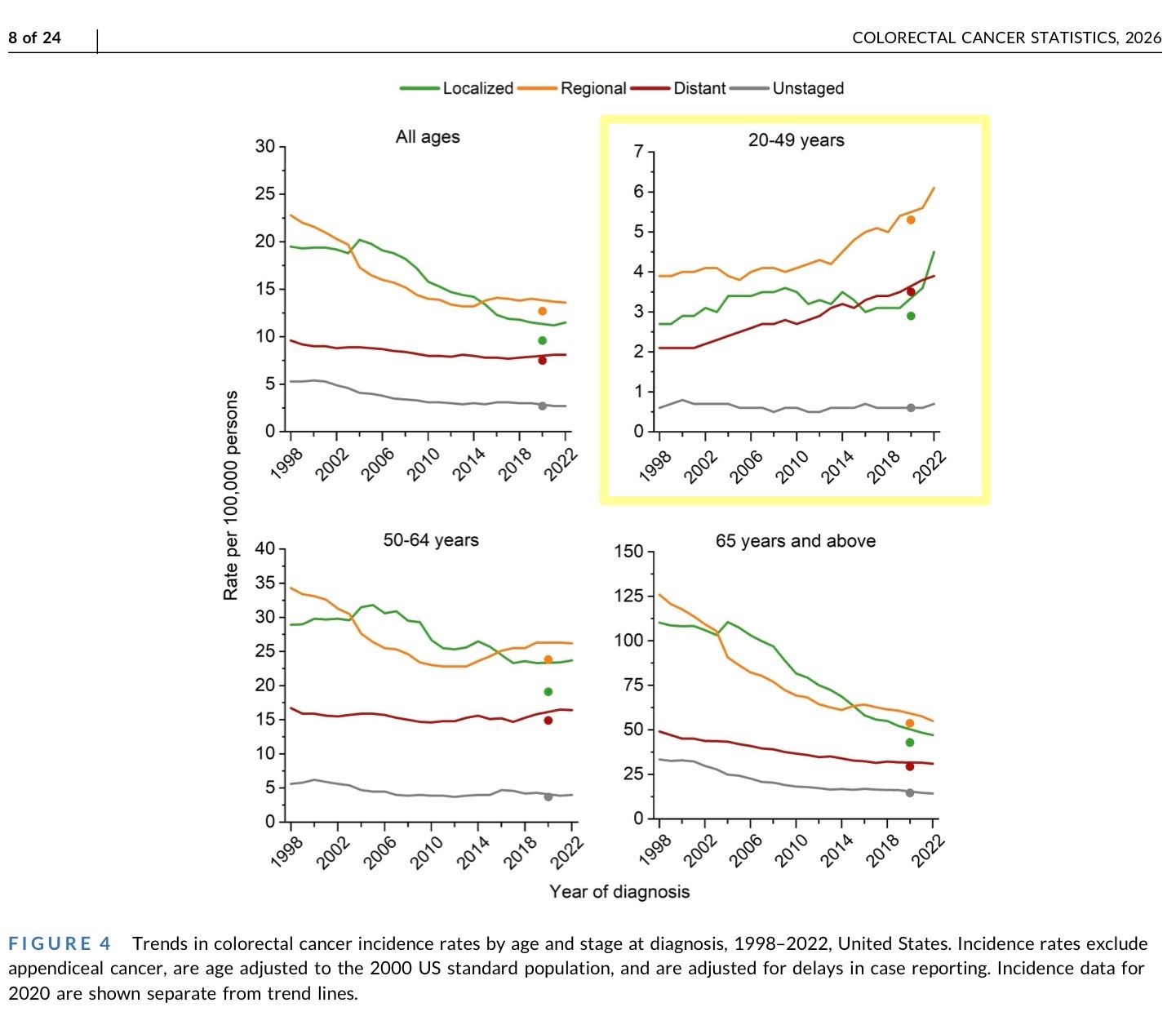
The incidence in adults aged 20–49 increased by 3% annually from 2013 to 2022, with mortality up 1% per year since 2004.
For adults 50–64, incidence is up 0.4% annually, and mortality has risen 1% per year since 2019, with the steepest increases seen in White individuals.
A critical issue is that younger patients are more likely to present with advanced disease—three in four are diagnosed at advanced stage, and 27% already have distant metastases at diagnosis.
Delayed diagnosis is common due to lack of screening, low symptom awareness, and health insurance barriers. Despite later stage at diagnosis, younger patients have similar or even better five-year survival than older adults, likely due to fewer comorbidities and more aggressive treatment, but they also face unique survivorship challenges, including fertility and sexual health concerns.
Racial and geographic disparities also persist. American Indian/Alaska Native individuals have the highest incidence and mortality rates, followed by Black individuals. Disparities are driven by differences in risk factor prevalence, access to care, and screening uptake.
What Can Explain This?
Traditional risk factors—obesity, physical inactivity, unhealthy diet, alcohol, and smoking—explain some but not all of the rise in early-onset CRC. The pattern is especially puzzling because the increase is most pronounced in rectal and distal colon cancers, while many risk factors are more strongly associated with proximal colon tumors. The report highlights emerging research on the gut microbiome, inflammation, ultraprocessed foods, microplastics, and antibiotic exposure as possible contributors. Only 16–20% of CRC in the under-50 group is due to inherited genetic syndromes, meaning the majority of cases are sporadic and likely linked to contemporary exposures.
A Note on the Birth Cohort Affect
The trend of rising CRC in young adults was first noticed in the 1990s. Data show that incidence began increasing in every generation born after 1950 in the U.S. and after 1960 in other developed countries. This so-called birth-cohort effect points to environmental and behavioral changes—likely involving diet, obesity, sedentary lifestyle, and possibly exposures like antibiotics or processed foods—that began decades ago and continue to shape CRC risk today.
The birth cohort effect: the phenomenon where the risk of developing a disease, such as colorectal cancer, is more closely linked to the year or period in which a person was born rather than their age at diagnosis.
The Tools We Have Now
Screening guidelines now start at 45 for average-risk adults, and the tools available to us have never been better. Here's where the technology stands:
Exact Sciences (Cologuard): Cologuard and Cologuard Plus are FDA-approved for adults 45 and older at average risk. These at-home tests detect DNA mutations and blood in stool, offering a non-invasive option for those hesitant about colonoscopy. Very high sensitivity (95%) for detecting Stage 1-4 CRC.
Guardant Health (Shield): Shield is the first FDA-approved blood test for CRC screening in average-risk adults 45+. It shows high adherence rates (over 90%) and good (but not the ideal) sensitivity (83%), making it a promising tool for boosting screening uptake among those unlikely to use traditional methods. However, it has limited detection (55%-65%) of Stage I colorectal cancer and does not detect 87% of precancerous lesions.
Freenome: Freenome is developing a multi-modal blood test for early CRC detection using machine learning and computational biology to analyze diverse biomarkers. Their PREEMPT CRC study is among the largest of its kind, aiming to deliver a more accessible and accurate screening option.
AI-Assisted Colonoscopy: AI has already transformed colonoscopy. Computer-aided detection systems use deep learning to analyze real-time video, highlighting suspicious polyps that might otherwise be missed. AI also characterizes polyps in real time—distinguishing benign from potentially malignant—which supports immediate clinical decisions and may reduce unnecessary biopsies.
Other Startups: Companies like GeneNews and Prevencio are exploring AI-driven blood and molecular diagnostics for CRC, while CellMax Life and others focus on globally affordable early detection tests.
Beyond screening and detection tools, generative AI can transform patient engagement. It could proactively reach out to patients about screening—or flag them earlier if there's a family history of CRC. GenAI could answer questions about different screening options and help patients choose what's right for them. Poor colonoscopy prep is also a real problem (I wrote about my own experience here!), so generative AI could guide patients through prep and ensure they're doing it correctly—ultimately improving screening quality.
Dashevsky's Dissection
This data lands differently depending on where you sit in the system.
For patients, the biggest gap is awareness. Most 40-somethings have no idea screening now starts at 45, let alone that they can do it with a blood draw or a stool kit at home. Generative AI has a real role here, too. It can answer questions and proactively reaching out, explaining the options in plain language, and guiding people through prep. The technology exists but adoption is the problem.
For us as (primary care) physicians, we need to screen our patients, recognize the red flags sooner, and have the conversation with younger patients who don't think they're at risk.
For health systems, the calculus depends on the payment model. If your patients are in a risk-based or value-based arrangement, catching CRC early is the whole game—it prevents the catastrophically expensive downstream costs of late-stage disease. The incentive structure already points in the right direction.
For those still in fee-for-service, the framing shifts, but the opportunity is still there. Blood-based and stool-based screening tests, as well as colonoscopies, are billable, increasingly covered, and genuinely useful. Deploying them proactively is both a revenue opportunity and the right thing to do for patients. Those two things don't have to be in conflict. Plus, if cancer is detected, you can refer to oncologists within the health system, capturing the full journey of care.
In summary, CRC in younger adults is accelerating, the tools to catch it early are better than they've ever been, and the incentives (clinical, financial, and moral) are aligned. We just have to act on them.